Attorneys in the Time of Cholera
This is the story of how lawyers are fighting the cholera epidemic in Haiti.
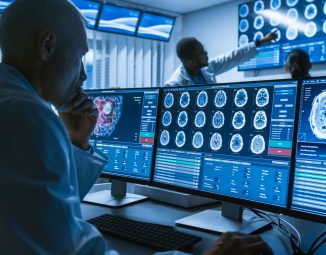
I am a physician with a subspecialty in infectious diseases. Since 2003, I have periodically travelled to Haiti to deliver basic medical care in underserved areas. I was also in Haiti two months after the earthquake that devastated the country and led to a quarter million deaths, reduced innumerable homes to rubble, abruptly terminated livelihoods and educations, and resulted in chronic disability for many.
In March, 2010, I worked at a field hospital about an hour outside of Port-au-Prince. Patients were assigned to each of about 50 large canvas tents, but each patient was accompanied by one or more family members, so conditions were crowded. The rainy season had not yet arrived, and it was hot, dry, and dusty. Many patients were immobilized by amputations or external hardware holding shattered bones in place. These sweaty conditions contributed to an already substantial risk for bacterial wound infections.
I met people whose responses to the earthquake were not just related to their physical injuries: one man unashamedly declared he was abandoning his wife because of the new large scar on her face; another man refused to go to a nearby clinic for removal of his infected metal rods until he was reassured that it was in a one-story building that was seismically-engineered; a pregnant woman receiving prenatal care for the first time learned she had HIV and she left the camp, abandoning her toddler to the category of “unaccompanied minor”; and someone stole a prosthetic foot.
In sum, the earthquake of January 12, 2010 left a population that was extremely vulnerable to many other traumas, besides the physical ones. So, when cholera was first introduced into Haiti in October 2010, the bacteria laid siege to an undefended population.
Haiti had plenty of waterborne dysentery-like illnesses previously, but a case of cholera had not been seen in over 100 years. Since cholera’s introduction nearly four years ago, 700,000 people have developed the severe diarrheal illness, and at least 8,500 have died.
How did this happen? In mid-October, United Nations (“UN”) peacekeepers from Nepal arrived at their base camp situated on the banks of Haiti’s principle river system in the Artibonite Valley. Days later, several Haitians, who lived downstream from the UN base, were carried to local clinics with profound dehydration secondary to copious vomiting and continuous “rice water” diarrhea, the classic description of cholera. Over the ensuing weeks, Haiti’s already taxed and partially destroyed health care system was overrun with patients.
Epidemiological and microbiological studies as well as forensic molecular technology showed that Haiti’s cholera strain is identical to the strain that is endemic (or commonplace) and often asymptomatic in Nepal. Associated Press and Al Jazeera reporters visiting the Nepalese base documented the UN workers dumping sewage where it flowed into the Artibonite River tributaries.
The UN’s own panel of independent experts has confirmed that the cholera outbreak coincided with the arrival of UN peacekeepers from Nepal, and that the strain of cholera present in Haiti is a perfect match with the strain in Nepal. The UN panel also reported that the Nepalese peacekeepers were not tested or treated for cholera prior to their deployment in Haiti, and that the sanitation piping on the base was cracked and haphazard. Finally, they confirmed the press reports that the base dumped their untreated human waste in open air pits that overflowed into the river when it rained.
Enter the United States-based Institute for Justice and Democracy in Haiti (“IJDH”) and its Haitian partner, Bureau des Avocats Internationaux (“BAI”), who together recognized the fundamental responsibility for this medical disaster lay with the UN. Both IJDH and BAI are small non-profit organizations made up of human rights attorneys. In Haiti, they have advocated for women who were victims of sexual assault and helped them face their perpetrators in court; they have also been instrumental in bringing Jean-Claude Duvalier (“Baby Doc”) to court for the brutalities committed during his regime as Haiti’s president during the 1970s and 1980s.
Now IJDH and the BAI are holding the UN accountable for the cholera epidemic and are suing for restitution. In November 2011, cholera victims, represented by the BAI, sought to invoke the settlement procedures that the UN had agreed to in international treaties, namely, that they agreed to provide out-of-court settlement mechanisms to victims of UN wrongdoing. The BAI submitted claims to the UN in a petition asking for: 1) a public acknowledgement of responsibility from the UN; 2) just compensation for the victims; and 3) installation of water and sanitation infrastructure needed to combat the ongoing epidemic.
The UN did not respond until February 2013 when it dismissed the claims as “not receivable,” because “consideration of these claims would necessarily include a review of policy or politics.” The UN refused to engage in mediation or discussion. Since there is no appeals process, Haitian cholera victims had no access to a mechanism that would result in justice.
As a result of the UN’s refusal to abide by the legal requirements of its own agreements, cholera victims filed a class-action suit against the UN in the Southern District of New York in October 2013. The case is pending, and the question of UN immunity is currently being briefed for the judge.
Cholera remains a very real threat to public health in Haiti, and the UN itself has warned that up to 2,000 people could die from the disease in 2014. This is because Haiti has a chronically inadequate water and sanitation infrastructure that is perpetuating the infection. Major rivers are used by the Haitian people for many daily purposes: drinking and cooking water, bathing and washing clothes. These open water systems continue to be contaminated by absent or flawed methods of handling human waste. The vicious cholera cycle will continue as long as this condition persists.
By the UN’s own definitions, the cholera epidemic in Haiti is a humanitarian crisis. But independent of the legal situation, the UN has not responded adequately to this crisis; to date, the UN has provided only 1% of the funding needed and repurposed another 9% from earthquake donations to install the water and sanitation infrastructure needed to control the epidemic. Sadly, some experts believe that cholera is now entrenched in and may never be eradicated entirely from Haiti.
From the medical perspective, cholera treatment clinics were set up across the country. Haitians have been educated about the symptoms and where to go—quickly—for treatment. Shipments of antibiotics, intravenous fluids, oral rehydration solutions, protective gloves and gowns continue, and a moderately effective cholera vaccine has been distributed to portions of the population. But none of this will stem the epidemic as long as water and sanitation are not secure. In addition, 75% of the cholera treatment clinics are now closed.
So, Haitians must now wait to learn if IJDH and BAI can control the cholera epidemic with legal argument, asking the UN to be accountable for the neglect and lack of appropriate supervision over health and sanitation practices that led to this humanitarian and health crisis.
Disclosures: Mary White is a supporter of IJDH and is a member of its Advisory Board. She was assisted in the writing of the legal details in this post by Brian Concannon, Executive Director of IJDH.
Mary H. White, MD is a physician evaluator in the Global Health Clinic at the Icahn School of Medicine at Mount Sinai, New York, NY. She is a graduate of Wellesley College and the Mount Sinai School of Medicine. She is board certified in internal medicine with a subspecialty in infectious diseases. She is a former attending physician at Memorial Sloan-Kettering Cancer Center and a former board member of Physicians for Human Rights and Partners in Health.